|
Nearly 9 in 10 rural counties in the United States now have at least one covid-19 patient.
Rural areas of the country, where 15 percent of Americans live, are seeing a rise in new daily cases even as the numbers decline in New York City and other urban centers that are now past their peak, according to Carrie Henning-Smith, a rural health researcher at the University of Minnesota School of Public Health. These new hot spots aren’t seeing the declines experts had hoped for, even after weeks of social distancing.
The shift is occurring even as state governors — both Democrats and Republicans — plan to restart economic activities in phases through the month of May, faced with unemployment claims so hefty some states are now seeking loans from the federal government to pay them. While many states haven’t met the qualifications for reopening laid out by the White House, President Trump is nonetheless cheerleading them in choosing to reopen.
Former FDA commissioner Scott Gottlieb:
|
 |
| |
Total covid-19 cases are still much lower in rural areas compared to cities. But they’re already growing at faster rates.
In the two-week period between April 13 and 27, novel coronavirus cases increased 125 percent in non-metro counties, compared to 68 percent in metro counties, according to research by the Kaiser Family Foundation. During that time period, deaths from the virus increased 169 percent in non-metro counties and 113 percent in metro counties.
The county with the most deaths per capita is Randolph County, Ga., with 278 deaths per 100,000 people (our colleagues have written deep-dive pieces about the area and how it has been ravaged by the disease).
It's not entirely clear why cases aren't being tamped down more quickly. It could be that people haven't socially distanced enough. The virus also took longer to spread to rural areas, so these places have been expected to peak later than the big cities.
“I think a lot of people are doing social distancing, taking this very seriously, but people still need to go out for work or running errands,” said Henning-Smith. “Eventually you can get a case in there and it starts to spread.”
Rural Americans lag behind urban and suburban dwellers on nearly every measure of health and wellness.
They tend to be older, earn lower incomes, have higher rates of unemployment and struggle with more chronic health conditions than the average person.
They live farther away from hospitals. Those rural hospitals typically have fewer ventilators, ICU beds and overall staff than urban hospitals. In the past decade, 128 rural hospitals have shuttered — three since the pandemic began. Half of all rural hospitals operate in the red.

Cristina Beltran inside the El Corral Cafe in Corona, N.M., a tiny town in rural New Mexico. (Damien Willis/Las Cruces Sun News/AP)
|
One might think urban residents would be at higher risk from covid-19, because they’re around dense crowds and public transportation more often.
But the pattern of flu deaths shows the risk of death is dramatically higher in the country’s thinly populated regions.
“Collectively, the 68 most rural counties of Kansas, for instance, have nearly 14 deaths per 100,000 people age 50 or older, well over double the rate for the county around Topeka (6.6), the state capital,” they wrote. “And the rate around New York City (3.4) is around half of that.”
There are unique challenges for rural people in marginalized communities. About one-third of Navajo Nation residents lack indoor plumbing, making it hard to carry out even the most basic preventive measure of hand-washing.
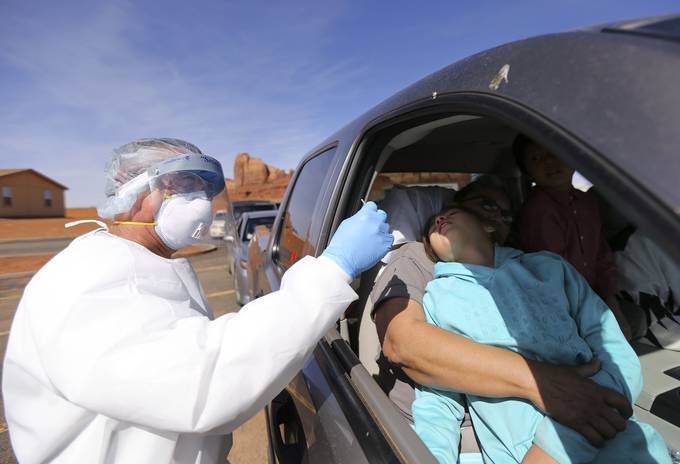
Vehicles line up for coronavirus testing outside of the Monument Valley Community Health Center in Oljato-Monument Valley, San Juan County. The Navajo Nation has one of the highest infection rates in the country. (Kristin Murphy/Deseret News/AP)
|
“Infection and death rates have ramped up in rural areas, particularly in the Deep South and other regions plagued by poverty,” she writes. “The Navajo Nation, for example, ranks close behind hot spots in the Northeast for infection rates.”
“Nobody is thinking about these pockets of vulnerability,” said George McGraw, founder and chief executive of the nonprofit DigDeep, who noted a “strong correlation” between the spread of the virus and communities that lack water.
|



No comments:
Post a Comment