|
Before coronavirus, policymakers were focused on eliminating another epidemic: opioid abuse. That's still a huge issue, and it's probably only going to get worse.
Yet centers that treat Americans with opioid addiction are being denied some extra emergency funds allocated by Congress — all because of a technicality.
These behavioral health centers — which serve nearly half a million people in the United States — are certified to provide medication-assisted treatment for opioid abuse that's approved by the Food and Drug Administration. This approach to addiction has been shown to be highly effective and has gained more acceptance across the country as states and localities sought over the past few years to lessen addiction's toll on their communities.
Now these substance abuse health providers are concerned about their financial state in an environment primed for increased struggles with addiction: The centers are anticipating a crushing wave of new demand amid the public health and economic crisis, even as they grapple with how to provide remote care.
The opioid oxycodone-acetaminophen, also known as Percocet. (Patrick Sison/AP)
|
Opioid treatment providers weren’t eligible to share in the $50 billion for Medicare providers from the Cares Act that lawmakers approved in March.
They are indeed Medicare providers: As of January, they were able to participate in the program. Congress made that change as part of the opioid response bill it passed in 2018.
But the Cares Act payments are based on 2019 Medicare payments. And opioid treatment providers didn’t get any Medicare payments that year, because they weren’t yet eligible.
To be fair, it's Medicaid — not Medicare — that is the country's biggest payer of addiction and mental- health services. Medicaid covers four in 10 people with opioid addiction.
But executives for these centers feel like they’ve been demoted from higher-priority health providers to more of an afterthought.
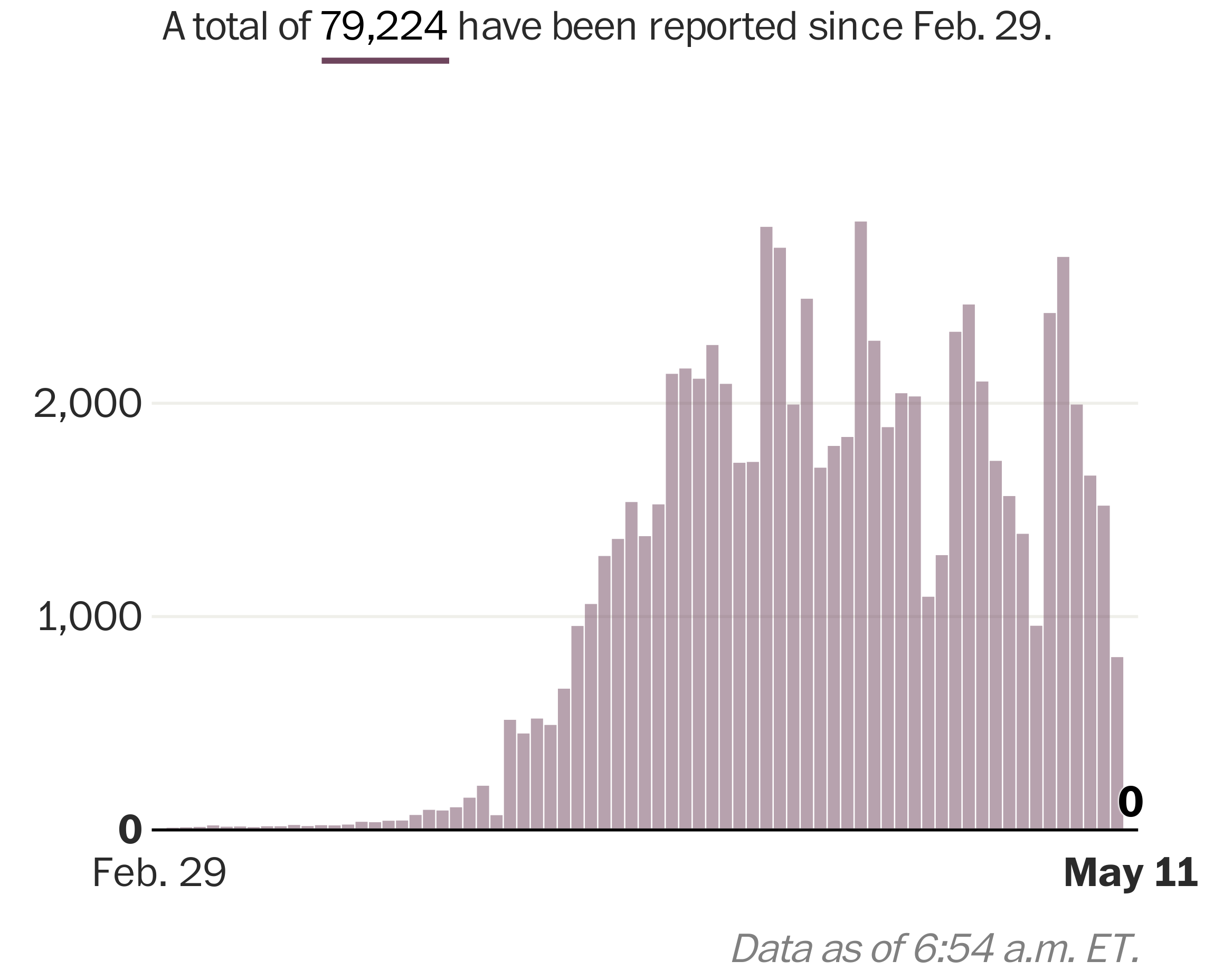
The coronavirus pandemic has killed nearly 80,000 people in the United States.
Before the virus struck, politicians and policymakers were wringing their hands over how to stem an opioid abuse crisis that has killed more than 400,000 people in the United States since 2000.
“Now is precisely the moment when we need to be supporting these kinds of programs that help folks who want to get into recovery,” Jason Kletter, president of BayMark Health Services, the country’s second-largest provider of opioid treatments, told me.
Experts predict the coronavirus crisis will lead more Americans to suffer from mental illness and abuse drugs and alcohol.
Some of the factors include increased isolation, stress and fear stemming from the pandemic.
In a report released Friday, Well Being Trust estimated 75,000 Americans could die from drug or alcohol misuse, or suicide, as a result of the pandemic.
“Heightened anxiety is a near-universal trigger for drug use, and it is difficult to think of a more stressful event — for all of us — than this pandemic,” wrote Peter Grinspoon, a doctor at Massachusetts General Hospital.
Kletter noted that “opioid use disorder is fundamentally a disease characterized by isolation and hopelessness.”
“There is evidence that epidemic is being exacerbated by this pandemic, so we need to make sure as a country we are continuing to provide recovery services to folks who need it to prevent a fourth wave of the opioid epidemic,” he added.

A fentanyl user displays opioid alternatives provided by the local health unit in Vancouver as those with addiction practice social distancing. (Jesse Winter/Reuters)
|
Congress hasn’t left substance abuse providers entirely out of its pandemic response bills, but the funding has been relatively meager.
The Cares Act provided $425 million for states to address mental illness and substance abuse, to be awarded by the Substance Abuse and Mental Health Services Administration at the Department of Health and Human Services.
“It was like a drop in the bucket,” said Chuck Ingoglia, president of the National Council for Behavioral Health.
Compare that to the $175 billion emergency fund Congress has set up for hospitals and other providers. Much of that funding has gone to hospitals directly caring for covid-19 patients. But other providers not on the front lines — such as orthopedic practices — also received dollars to help make up lost revenue when they were forced to suspend nonessential services for weeks on end.
Substance abuse providers stress that they’ve also suffered financial losses.
Six in 10 community behavioral health organizations believe they can survive financially no longer than three months amid the pandemic, according to a survey released last month by NCBH.
The council and the American Society of Addiction Medicine have asked Congress for $38.5 billion in emergency funds for behavioral health organizations “to avert a large-scale public health calamity.” They want much of the funding awarded through the Medicaid program, considering the outsize role it plays in paying for treatment for people who abuse opioids.
“This pandemic has spread fear and anxiety across our nation, leaving no one unaffected,” the letter said. “Our mental health disorder and addiction treatment providers are facing an influx of need.”
| 



No comments:
Post a Comment